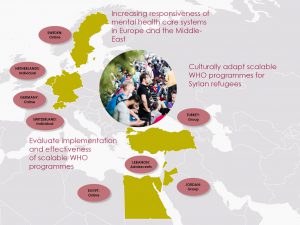
 Rapid appraisal of health systems
Rapid appraisal of health systems
A total of 13 million Syrians have been displaced by the ongoing conflict in Syria. The majority has found refuge in neighbouring countries, while countries in Europe also accepted large numbers of Syrian refugees. Refugees are often vulnerable to psychosocial distress because of exposure to war and violence, traumatic events experienced during the flight from Syria and the stress of settling in a new country. For some refugees, this may manifest in post-traumatic stress disorder, depression and/or anxiety disorder if they remain untreated. Many host countries are ill-equipped to respond to the large number of Syrian refugees who may need to access comprehensive mental health and psychosocial support (MHPSS) services. The STRENGTHS study has been initiated to develop effective strategies for scale up effective low intensity mental health interventions that can help to meet these needs in settings where resources are limited.
For this study, a rapid appraisal (RA) has been done to assess the responsiveness of the health care system to the psychosocial needs of Syrian refugees in all partner countries. The assessment examines the way Syrian refugees with mental health needs navigate the health care system.
Methodology
A number of methods are used for the RA. First, desk-based studies were conducted to collect information about the structure of the health system and any bottlenecks to implementation of effective interventions. Second, analysis was done of existing qualitative data collected by STRENGTHS partners for their formative intervention work. Third, a series of semi-structured interviews will be conducted in the next 18 months among: key informants such as government officials and policy makers; MHPSS providers; and Syrian refugees receiving care and their family members in the STRENGTHS study countries.
The RA is a work in progress. The following are some brief initial findings for each of the STRENGTHS study countries:
Egypt
Initial findings suggest high mental health needs among Syrian refugees in Egypt, albeit based on limited evidence. Our findings also indicate that the ‘parallel’ health system (i.e. NGO services) are the primary route for Syrian refugees to access mental health as they are more accessible. Treatment for PTSD and other mental disorders are available in the public sector but is expensive. Given these circumstances, the free online mental health services being developed by STRENGTHS seem to be a good option for Syrian refugees.
Germany
Initial findings suggest the German mental health care systems offers adequate treatment for German nationals. However, there seems to be a substantial inequity in access when it comes to treatment for mental disorders for refugees. Access to psychotherapies is restricted within the first 15 months of residence. This may lead to delayed diagnosis and late treatment onset which may exacerbate the severity of symptoms. The literature indicates that Syrians enjoy the full range of health care options after the 15 months waiting period but still face socio-cultural barriers to accessing care.
Jordan
Initial findings highlight barriers in accessing mental health services for Syrian refugees in Jordan. These include acceptability barriers (e.g. linguistic, cultural, and attitudes of health services users and providers), availability, geographic accessibility and affordability. These barriers need to be further investigated, especially from the perspective of Syrian users of mental health services.
Lebanon
Initial findings suggest an adequate number of mental health facilities available at the tertiary level but inadequate resources at the community and primary health care level for Lebanese nationals. Mental health care for Syrian refugees is predominantly provided by NGOs which challenges the sustainability of service provision in the future. Furthermore, it was found that there is a lack of communication between the different providers operating at the public and parallel health system, and that within the parallel health system coordination of care and pathways of care can be improved. The implementation and scaling up of MH-GAP faced challenges and needs to be investigated further as it may provide important information about the scaling up of PM+.
Sweden
Initial findings from the rapid analysis suggests that Syrian refugees refuse or delay care-seeking due to limited knowledge of mental health care, somatization, and stigma. Health screening for asylum seekers seems to insufficiently address mental health, hampering early detection of psychological issues. Initial findings also indicate a lack of health centres and providers specialized in refugee and/or trauma care in rural areas in Sweden. Consequently, Syrian refugees may experience physical access barriers and do not receive culturally appropriate care.
Switzerland
Initial findings indicate acceptability of care is one of the main obstacles for Syrian refugees hampering access to health care in Switzerland. Distrust in the system and in health care providers has emerged as a key theme. This calls for the need to educate Syrian refugees about the mental health care system and care options to decrease mistrust. Cultural awareness training for Swiss health care providers seems to be equally important. Syrian refugees might be more drawn to PM+ since the programme of care is delivered by lay health care providers (Syrian Refugees themselves). However, distrust of Syrian refugees in the Swiss health care system may remain and might need to be addressed during the implementation of PM+.
The Netherlands
Initial findings indicate that acceptability barriers are key for Syrian refugees in the Netherlands. Results from the literature confirm findings of the cultural adaptation phase and indicate that PM+ providers will likely be acceptable to patients. However, findings also suggest that some Syrian patients may distrust providers from their own country. Integration of PM+ into the public health system would require treatment to be covered by health insurers to be financially viable, but insurance companies do not commonly cover services provided by those who are not professionally registered. Another option is for PM+ to be offered outside the public health system. The cost-effectiveness and financial sustainability of scaling up PM+ will therefore be critical.
Turkey
Initial findings depict a situation in which services are made available for refugees. However, access falls short because of poor acceptability and financial barriers. Another key point was the lack of treatment demand among the Syrian population. There also seems to be inequity in access to health care when it comes to the difference in temporary protection status of refugees.
Next steps
The RA will be updated with findings from qualitative interviews that will be conducted over the next 18 months with: key informants such as government officials and policy makers; MHPSS providers; and Syrian refugees receiving care and their family members in the STRENGTHS study countries.


